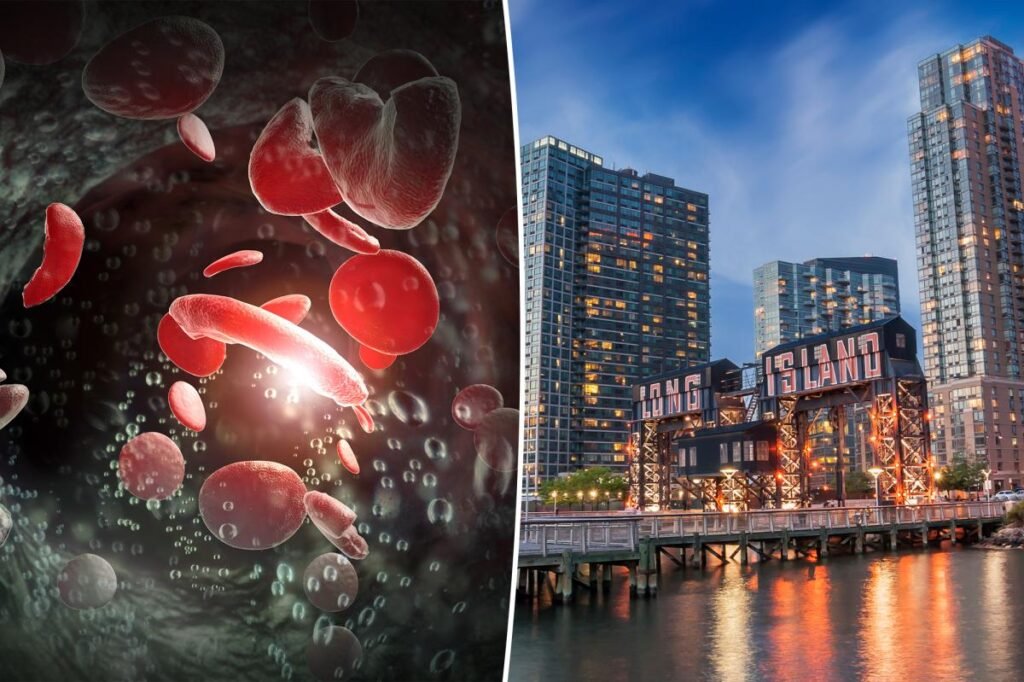
About 100,000 Americans have sickle cell disease (SCD), the most common inherited blood disorder in the US.
Roughly 10% of patients reside in New York State, with the majority living in NYC, researchers at NYU School of Global Public Health found.
Using data from 42,200 SCD hospitalizations in the state between 2009 and 2022, researchers assessed the length of hospital stays, total charges, severity of illness and risk of death.
They found that while NYC had the most SCD hospitalizations, Long Island had the highest percentage (10%) of hospitalizations with a major risk of death.
“This suggests a high sickle cell disease burden on Long Island,” study author Emeka Iloegbu said in a statement. “Long Island and New York City had high costs, which may suggest that these regions are managing clinically complex cases or have differences in specialized care or care-delivery practices.”
SCD is caused by a mutation in the gene responsible for making hemoglobin, a protein in red blood cells. This mutation is most prevalent among people of African descent, according to Johns Hopkins Medicine.
The mutation leads to crescent-shaped blood cells that can’t effectively carry oxygen through the body, so people with SCD face risks of organ damage, anemia, strokes, infections and excruciating pain.
These complications send patients to the hospital, where they experience a wide range of care.
“A range of factors can influence care for sickle cell disease — whether people are experiencing multiple health conditions at once, whether hospitals have a dedicated sickle cell disease team with hematologists with specialized training or have protocols in the emergency department for people who present in crisis,” said Iloegbu.
The NYU study reported that within the state, central New York had the longest average hospital stay (6.3 days), followed by the Hudson Valley (6.2 days).
NYC had a shorter length of stay on average (5.5 days) and fewer patients at major risk of death.
The study also found that Long Island had the highest total charges for hospital stays.
Living with SCD can be costly: One study noted that privately insured individuals face an estimated $1.7 million in lifetime SCD medical costs, with roughly $44,000 in out-of-pocket charges.
Most people hospitalized in New York (83%) were black. Adults 18 to 29 years old accounted for the largest share (40%) of hospitalizations, followed by those aged 30-49 (32%).
Researchers believe these statistics reflect a failure in appropriately transitioning SCD patients from pediatric to adult care.
Meanwhile, the percentage of “major severity” hospitalizations increased dramatically, from 13% in 2009 to 27% in 2022. During the same period, hospitalizations classified as “major risk of mortality” rose from 3% to 13%.
The researchers attributed the spike to COVID-19 complications and the pandemic disrupting care.
The findings were published Friday in JAMA Network Open.
Researchers believe their findings can improve care for those with SCD.
“Understanding regional differences in sickle cell disease can help us to identify and address gaps in care,” said study author Emmanuel Peprah.
For researchers, addressing those gaps includes improving access to specialists and educating providers about therapy options.
The team also believes that prioritizing SCD funding, updating public health policies and increasing availability of effective therapies could reduce the burden on emergency departments.
In 1975, New York State implemented the first SCD newborn screening program in the US. This testing supports early diagnosis and intervention, both of which can significantly improve health outcomes.
The study authors noted that migration patterns have shifted and many people seeking SCD care in New York were not screened as infants.
“Instead of being screened and monitored, the entry into the health system for these individuals is the emergency department,” said Iloegbu. “Knowing that certain regions of New York have increased severity or longer lengths of stay could contribute to the need for improved surveillance, especially at the patient level.”
While Long Island bears a “high” burden of SCD, it is also leading the way in treatment options.
Last year, a Long Island hospital administered a life-changing gene therapy treatment and wiped out SCD in a local man.
Read the full article here